Executive Summary: Food Insecurity Is Associated with Mental Health
Executive Summary: Food Insecurity Is Associated with Mental Health
Food insecurity is a problem beyond empty fridges and pantries. Evidence from the early days of the pandemic in the United States suggests that food insecurity is associated with depression, anxiety and stress.
These mental health problems were more prevalent among those with greater food insecurity and younger adults 18–39 years of age, those with children and adults working full or part-time. For children, food insecurity is also associated with poor academic performance. A link between hunger and mental health has always existed, but the pandemic has made this so much worse.
The national survey was taken during March 19 – 24, 2020, and revealed that food insecurity was associated with a higher likelihood of being extremely or very concerned about the effect of the virus on health, income, daily life, the economy, and the ability to feed one’s family. During this time, the mental health of low-income adults in the United States was already poor, with disproportionate rates of depression, anxiety and stress among food-insecure households.
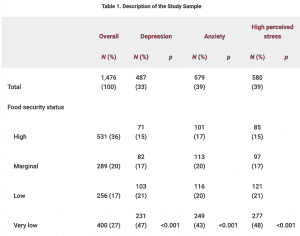
While the relationship between food insecurity and mental health is not new, the study suggests that COVID-19 presents a new set of conditions that potentially exacerbate that dynamic. A majority of low-income adults shared worries about the effects of COVID-19 on the economy in general no matter their food security status. However, there were clear disparities based on food security status in concerns about the effects of the pandemic on one’s income, daily life and ability to provide food for one’s family. On top of depression, anxiety or stress related to living with food insecurity itself, the pandemic is inducing stressful circumstances that influence the disparity in the rates of depression, anxiety and stress correlated with food insecurity.
The study further suggests that inequity within the negative mental health impact of the pandemic on the most vulnerable individuals of our community will require urgent attention. Evidence shows that psychological distress, including post-traumatic stress disorder, depression, anxiety and other mental health outcomes, escalates after large-scale disasters including epidemics such as the SARS outbreak in 2003. It is notable that during March 2020, mental health among low-income food-insecure adults was already low. The mandated social distancing and isolation heightened loneliness and depression on top of the usual stress and anxiety around financial uncertainty and health concerns.
It is essential that the health care system plan for increased demand for mental health care services in short and long term scenarios and develop ways to address care in the context of the pandemic and prioritize equitable access to services for low-income individuals. It is also suggested that mobilizing nontraditional resources within the community offers preventative mental health services and fosters traditional models of support and care. This type of outreach could be crucial to low-income, food-income populations who might have lost health insurance benefits and who are reluctant or resist the formal health care system or those who are pushed to choose between food and medicine.
It is also noted that policies to mitigate and prevent food insecurity can substantially benefit mental health by unburdening those experiencing stress and anxiety about practical concerns tied to being food-insecure. Expanded Supplemental Nutrition Assistance Program (SNAP) benefits are essential to continue to support struggling households through and beyond the pandemic. Previous data show lower rates of depression among low-income SNAP participants. On top of expanded SNAP benefits, direct income support, extended unemployment benefits and increased emergency food assistance and resources could help low-income families get through the pandemic while providing positive, additional benefits for mental health over the long term.
Open Responses in the Study to “Is There Anything Else You Would Like Us to Know About How You Are Dealing with the Coronavirus, and How It Is Affecting Your Life?”
“I have lived week by week, just barely, to avoid asking for help. Now I am falling through the cracks, invisible to a system suddenly flooded by the needs of people it already recognizes as needing help. I am in danger of losing my home and everything in it. I am very scared.”—Adult with LFS
“I have anxiety disorders, so this is worse on me. Every sniffle or runny nose which I usually think are my allergies or sinusitis … I now think is a death sentence. I am a nervous wreck anytime I have to go anywhere.”—Adult with MFS
“I’m low income so even missing one day could make me and my family go hungry for a week so we are suffering because other people got sick even though we are healthy.”—Adult with VLFS





